
Headmaster with chalk
Headmasters use school fees to purchase supplies and pay school expenses. At one school, people had so little money for fees that the headmaster could afford to purchase just three packs of chalk with 50 pieces per pack. He gave each teacher two sticks of chalk per day, telling them that when the chalk runs out, they would have to teach without using the blackboard. The students themselves have no pencils, pens, notebooks or books (although the school had books that students could use there).
People in the hospital’s catchment area are impoverished and generally poorly educated. Unemployment nationwide was 90% and inflation was calculated to be sextillion percent in January. In late January, the Zimbabwe government declared the nation’s currency to be worthless and abandoned it – it was by then issuing bills for ten trillion Zimbabwe dollars. The government decreed that trade was to be conducted using U.S. dollars, euros, South African rand, the Botswana pula or the Mozambique metical. Dollars, euros and rand were preferred. Word spread that people needed “oo-sa” dollars (U.S.A. dollars). People in rural areas in particular didn’t know what usa dollars were or where to get them, yet they needed them to pay school fees and purchase seed and fertilizer (which were often unavailable even for those with money) and other commodities. Nor did people know the value of “4-ex” (foreign exchange) currencies, so they didn’t know whether $3.00 for a loaf of bread was fair or not – and neither did the merchants. This led to confusion and exploitation. “A person can work like a donkey and be paid very little,” hospital director Dr. Elizabeth Tarira, said.
I also joined Melania as she drove to villages on the escarpment and to Muzarabani in the Zambezi valley to meet with groups of hospital-trained, volunteer, home-based care workers and with groups of HIV+ people who provide HIV education, promote counseling and testing and encourage positive living in their communities. She helped these groups with problems and passed out donated clothing. The home-based care workers received new kits donated by World Vision that contained soap and a towel, pens and a notebook, a flashlight and batteries, and other supplies to help them with their home visits.
Hunger increases child abuse
The growing season, which ended in March, helped to ease widespread food shortages, hunger and starvation. But in many areas, wild grass was growing instead of maize. These areas were left unplanted, I was told, because people had no money and because seed and fertilizer were often unavailable.
Hunger remained a serious problem, and it led to child abuse and to an increase in the number of burn cases at the hospital. Zachao, an 8-year-old orphan being raised by elderly grandparents, is one example. He was driven by hunger to steal from a neighbor’s farm plot. He tore ears of maize from the plants and ate them raw, and pulled groundnut (peanut) plants from the ground and ate the green, immature nuts right there in the field. He’d done this several times, and had been scolded by his grandfather for it. The grandparents were being harassed by villagers because of the boy’s actions, and the neighbor threatened to leave poisoned produce out to kill the child. Desperate, the grandfather wrapped the child’s hands in plastic and set it on fire. He hoped the drastic action would stop the boy’s behavior and appease the neighbor’s anger (it was said that people were harrassing the old couple and tearing out their few crops in retribution, leaving them – and the child – with even less to eat).
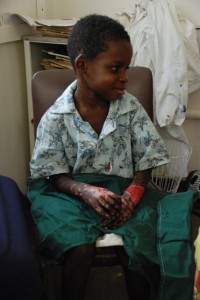
Zachao
Another instance involved a boy who’d stolen some of his family’s wheat and ate it. His father burned his hands with a coal to punish him for stealing and put the coal to his forehead to punish his head for thinking of stealing. In another case, a grandmother punished her granddaughter for taking an ear of maize and roasting it in a pan by holding the child’s hand down on the hot pan. These children, all 8-10 years old, were being treated by Dr. Julia at the hospital to the degree possible with limited supplies. The hospital’s physical therapist was working to maintain flexibility of their hands and fingers during healing.
Elizabeth wrote an impassioned letter about these cases to several newspapers – blaming hunger and despair for the problem. A number of papers covered the story. The government paper, The Herald, blamed the grandparents for not controlling their children. An independent paper, The Standard, attributed the problems to hunger, which they said was killing people in their huts. The doctors at St. Albert’s wondered among themselves how many similar cases were going unreported in the villages.

A St Albert's rehabilitation specialist working with Zachao
(St. Albert’s treats a considerable number of burn patients, many of them epileptics. The disease is often poorly controlled because the medicine can be hard to find. People in the villages usually cook over open fires. St. Albert’s sees many epileptics who have had a seizure beside an open fire and passed out with a hand, arm or leg lying in the fire.)
The hospital has many needs. I visited the maintenance department where two mechanics work on the hospital vehicles, farm equipment, maize grinder and other equipment. They need an arch welder. Yet, in spite of the many problems, Elizabeth has amazing successes, too. The farm project is going strong, though she has had to hire guards to protect the field from pilferage, and the new water filtration system enables the hospital to use water from the reservoir. Elizabeth wants to expand the filtration system so she can supply the entire mission, which includes a primary and secondary school (a boarding school), as well as the hospital. In addition, Elizabeth is helping her sister, Juliet, continue a program for desperate young pregnant women.
The Shelter Trust
Juliet lives in Harare and runs the Shelter Trust, which provides temporary housing for young pregnant women abandoned by their families because of their pregnancy. These women are often despondent and suicidal and have no where to turn. In better days, the Trust housed up to 12 women, offered training in sewing and other income-generating work, and provided prenatal care and safe delivery of the baby. Juliet has a Masters in social work, and, Elizabeth said, could find a good job with one of the nongovernmental organizations working in Zimbabwe, but she won’t because she wants to keep the Shelter open. She survives with the help of her daughter, also a university graduate, who still had a job at a bank.

Juliet at her desk at the Shelter Trust
Juliet keeps the Shelter Trust going through sheer will. She no longer receives funding from businesses or the government. Gone are the staff and the training classes for the women. She runs the program alone, with no income or budget. St. Albert’s has stepped in to provide prenatal care and deliveries. Elizabeth travels frequently to Harare to conduct business (necessary because the phone system serving the hospital has been down for years), and she uses those trips to help the Shelter. A nurse from St Albert’s will ride with Elizabeth to the Shelter to provide prenatal care and education. Women who are near term then ride with her back to St. Albert’s and stay at the hospital’s mother’s shelter until delivery. After the baby is born, the mother and infant return with Elizabeth to the Shelter Trust, where Juliet works to reunite them with the mother’s family or a relative (it’s harder for families to reject a young woman with a newborn).
Delivery is a problem for pregnant women in Harare. Pregnant women who go to a clinic or hospital to deliver must pay $50+ and bring the materials needed for the delivery, such as four or five pairs of disposable gloves, suture material, umbilical cord clamp, and cotton swabs and gauze.
I was talking with Juliet on one occasion before Elizabeth and I were to return to St. Albert’s. We were to take three young pregnant women with us, but one of the three began going into labor. Elizabeth examined her and found she was hypertensive and would likely experience a complicated delivery. She would have to remain in Harare. Juliet had no money, and the clinic would charge $50 for the birth. More likely, the clinic would want the woman taken to the hospital, which would cost more. Elizabeth gave Juliet two $50 bills to help with the expense, and we drove off with the two other women.
Elizabeth wrote later to describe the outcome:
“Just a line to tell you that the woman whom we left at Shelter Trust was not accepted at the clinic. She was then taken to Harare Central Hospital where she delivered around 8:00 pm. If we had carried her in the car with the many potholes along the roads she would have delivered earlier. Of course there was the issue of paying. At the Hospital for a normal delivery they wanted 270 US dollars, which of course Juliet did not have. She took out only 50 dollars, keeping the other 50 for another emergency, but the balance bill will follow her later. This is how life goes on. Cecilia was still at the Shelter. I do not know when the child will be adopted as yet. Hopefully the baby will turn out to be negative for HIV since the mother is positive.”
Cecilia was a young, pregnant woman who came to the shelter, delivered at St. Albert’s and returned to the Trust with Elizabeth the day I returned to the U.S. She was epileptic and wanted to give her baby up for adoption. Elizabeth wrote in April that Cecilia had decided to keep the baby.
The Social Welfare Dept. made “a lot of unrealistic demands from her, but the whole issue was that they could not have a child born from an HIV-positive mother be adopted. They would not find a foster parent. About that other woman who delivered at Harare Central Hospitals, the actual figure they wanted for normal delivery was 290 US dollars. Too much actually.”
Florence
Though I was already home, my thoughts on Wednesday, March 18, were back at St. Albert’s with Florence, a 10-12 year old patient who came from a village 25 kms from the hospital. An infection in her lower leg had spread to her tibia, causing osteomyelitis. The bone grew weak and cracked and a fragment pushed out through the front of her leg. The break and protrusion from the skin seemed to cause her no pain. Her mother, unaware of the seriousness of the problem, hoped the injury would heal on its own. Neighbors finally brought the child to the hospital. By then, the lower leg required amputation to prevent the infection from spreading to her upper leg. The mother walked to the hospital later to be with her daughter – which meant that her garden, needed for food, would go untended.
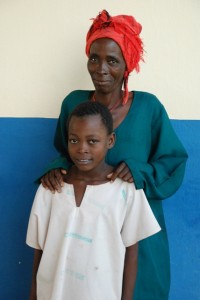
Florence and her mother
Zimbabwe’s cholera epidemic had eased before I arrived. St. Albert’s had one patient in their isolation area – a couple of white tents set up adjacent to the hospital grounds with shallow pits in the ground lined with a plastic sheet and containing a disinfectant that one walks through when entering or leaving the isolation area. Clinics had similar cholera isolation areas.
Last, because of Zimbabwe’s economic collapse, Elizabeth receives no money from the Zimbabwe government or from the Catholic diocese to keep the hospital running. She relies on Providence – and on donations from friends of the hospital. She says her fund-raising efforts should qualify her for a “Beggar of the Year Award.” Please keep in mind that even small donations to the hospital add up. They help Elizabeth keep St. Albert’s running and remind the doctors and staff that they are not forgotten.
Darrell

Darrell,
Very tough situation there. I really am proud of all you are doing to assist these people.
Gary